The COVID-19 pandemic has killed millions of people worldwide and led to devastating economic impact. A vaccine is one of the biggest hopes for stopping the pandemic.
The World Health Organization (WHO) is working with multiple stakeholders to ensure groups at higher risk of becoming infected and dying (e.g. elderly people and healthcare workers) receive a safe an effective COVID-19 vaccine in the next six months.
The WHO’s Director-General asked your help to build a plan to achieve this goal. What should be included in this plan?

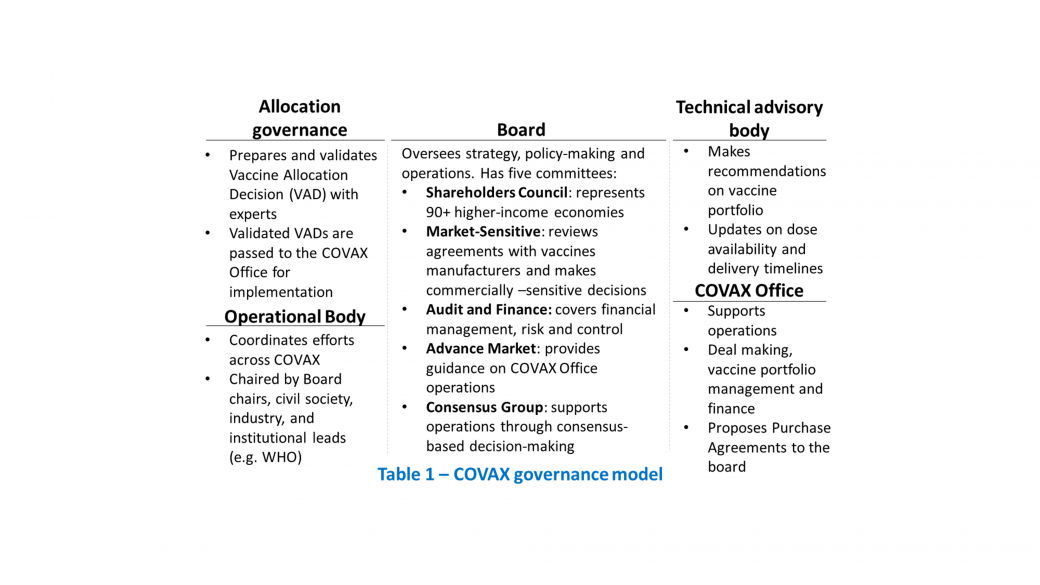
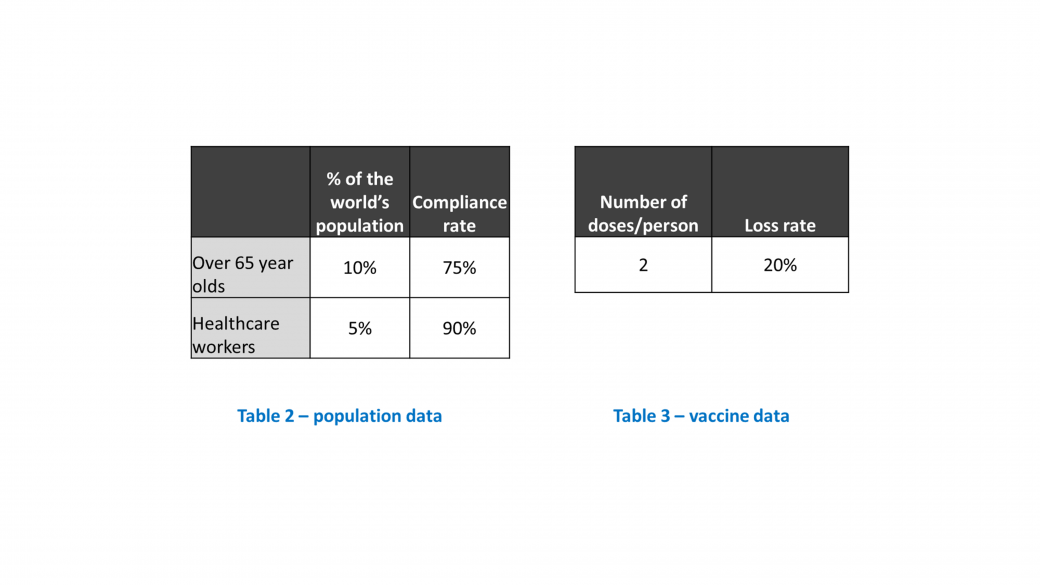
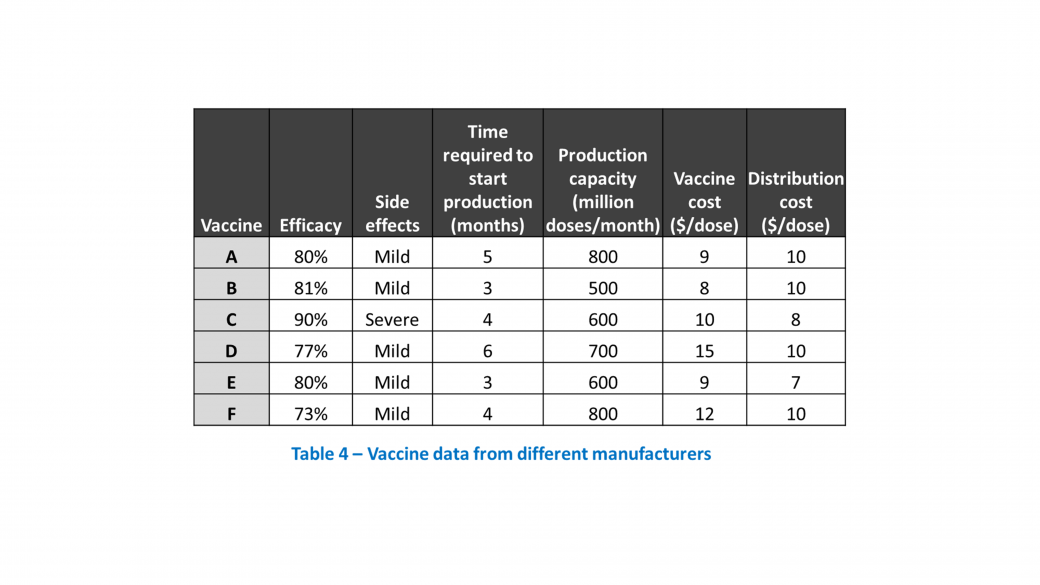
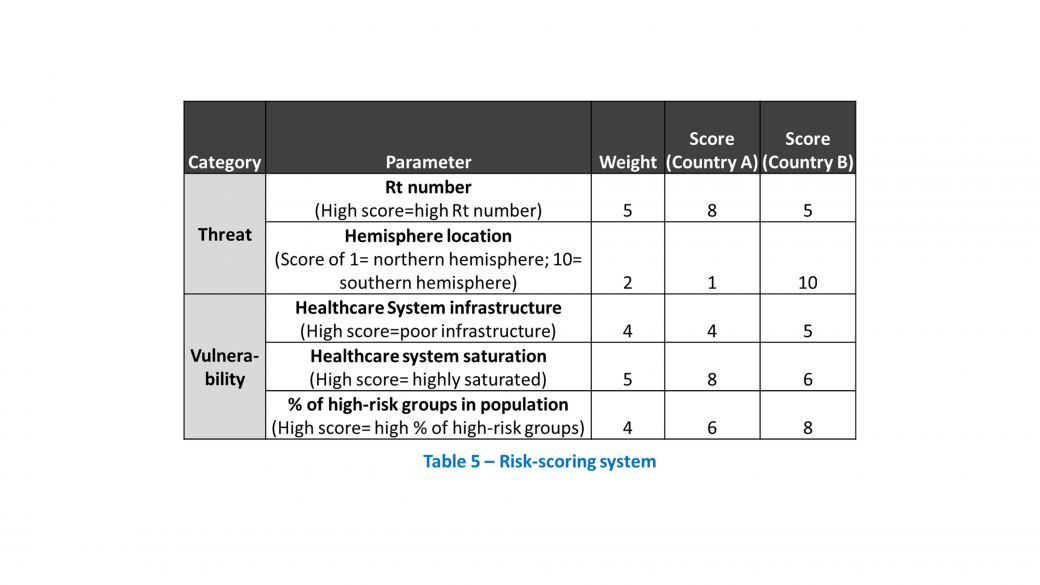

MBB Case: COVID-19 Vaccine
i